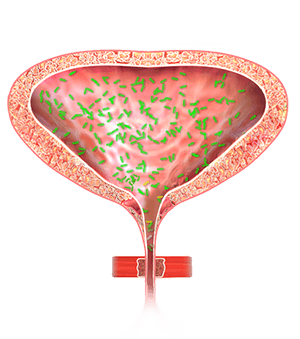
A urinary tract infection (UTI) is the infection of the urinary system which mainly includes the kidneys, ureters, bladder, prostate (in men) and urethra. Urinary tract infections usually occur when bacteria migrate up the urethra into the bladder.
Normal urine contains no bacteria (germs). Bacteria can get into the urine and the urinary tract from the skin around the rectum and genitals by traveling up the urethra into the bladder. Lower urinary tract infection or cystitis is the bacterial infection which is confined only to the bladder and the urethra.
Upper urinary tract infection or Pyelonephritis is a bacterial infection of the kidneys resulting from bacteria traveling from outside the body into the urethra to the bladder and finally to the kidneys through the ureters.
For women, the risk of having a UTI is greater than in men. This is probably because of a shorter urethra, making it easier for bacteria to arrive in the bladder. Bacteria can get into the urinary tract following sexual intercourse or use of a diaphragm for birth control. Other risk factors include diabetes, immunocompromise (such as HIV infection or steroid use), and menopause.
Recurrent urinary tract infections are defined as having two or more infections within 6 months, or three or more infections within a year. These infections should be proven by urine culture.
Risk Factors
The following risk factors increase the likelihood of having a urinary tract infection:
- Diabetes
- Advanced age
- Urinary retention (difficulty fully emptying the bladder)
- Use of urinary catheter to urinate
- Having urinary tract abnormalities that block the flow of urine
- Bowel incontinence (the loss of bowel control)
- Kidney stones
- Pregnancy
- Surgical procedures involving the urinary tract
Symptoms of UTI
If you have cystitis or bladder infection you may have an intense urge to pass urine, pain or burning sensation when urinating, and urine may look cloudy, bloody or have a foul smell.
If you have Pyelonephritis or kidney infection you may have a fever with chills, flushed, reddened skin, pain in the back, nausea, and vomiting.
Diagnosis of UTI
Your doctor will ask about urinary symptoms and then order the following tests if a UTI is suspected.
Urine Test
A sample of urine is collected and analyzed in a laboratory to determine if pus, red blood cells or bacteria are present.
Ultrasound Scan
An ultrasound scan is a non-invasive, painless scan done to see whether there are any abnormalities in your urinary tract, such as a narrow ureter or a bladder stone or kidney stone.
Cystoscopy
In cystoscopy a flexible camera is placed into the bladder through the urethra. This procedure is done in the office and can diagnose conditions that can cause recurrent infections, such as debris in the bladder, incomplete emptying of the bladder due to anatomic anomalies, or fistulous connections to other organs.
DMSA Scan
A Di-mercaptosuccinic acid (DMSA) scan is a scan that is used to assess the state of the kidney. It is occasionally done six months after and episode of pyelonephritiswith unusual symptoms or after several recurring UTIs. During this procedure, DMSA will be injected into your body. The DMSA will start building up inside the kidneys after an hour. A series of pictures of your kidneys are then taken with a gamma camera. This scan takes about 30 minutes to complete.
Voiding cystourethrogram (VCUG)
This test is used to study the bladder and to check for Vesicoureteral reflux. During MCUG, you are asked to lie on a bed with a urinary drainage catheter in place. A contrast agent is injected into the bladder through the catheter. An X-ray film will be taken as the contrast agent passes out of your bladder. If the X-ray film shows that the contrast agent is leaking back up the ureters to the kidneys from the bladder then Vesicoureteral reflux is diagnosed
Treatment of UTIs
While you are experiencing a urinary tract infection antibiotics are usually prescribed. It usually takes 2-3 days of antibiotics for symptoms to improve. Always complete the full course of antibiotics you are prescribed. If you stop taking antibiotics before completing the course, you run the risk of training the bacterial in your infection to be resistant to that type of antibiotic.
Prevention of UTIs
Behavioral Approaches
For some patients, certain behaviors can trigger urinary tract infections. These can include not drinking enough water, vaginal cleaning products, use of certain sexual lubricants, self-catheterization, and others. Your physician can help you to identify behaviors that might be triggering infections for you and how to manage them.
Dietary Supplements
Some dietary supplements have been shown to reduce the risk of urinary tract infections. Cranberry supplements in general have been shown to be effective, although few specific products have evidence to support them. Probiotics, lactobacillus, and prebiotics have not been found to be effective therapy for preventing UTIs, although many patients choose to use them. This is an area that is ripe for future scientific research.
Medications
Your doctor may recommend medical therapy to prevent urinary tract infections. This may include suppressive, self-start, or prophylactic antibiotics, or other antibacterial medications such as methenamine hippurate. Your physician will try to minimize the amount of antibiotics you require to reduce side effects. Always take your antibiotics are prescribed and don’t “save” antibiotics for future use unless directed.
Post-menopausal women often benefit from intravaginal estrogen cream. If your doctor prescribes intravaginal estrogen cream, apply it as follow: One pea sized dollop nightly for two weeks, and one slightly smaller dollop three nights per week thereafter.
