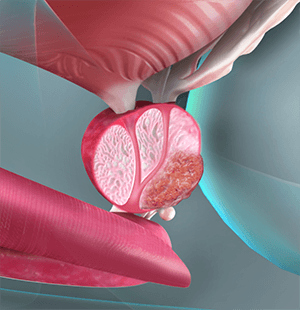
What is Prostate Cancer?
Prostate cancer is the most common cancer found in men. It is estimated that the risk of a man being diagnosed with prostate cancer by his 85th birthday is 1 in 5.
Prostate cancer is the second leading cause of cancer death in men, yet it is highly curable if discovered while still confined to the prostate gland. Most prostate cancers grow slowly, usually remain confined within the prostate gland and cause no harm. This type may need minimal or no treatment other than close surveillance. Some prostate cancers, however, are aggressive and can spread quickly, early detection has a much better chance of successful treatment.
Causes of Prostate Cancer
Prostate cancer causes no signs or symptoms in its early stages. Symptoms may show once cancer grows and spreads to other parts of the body. Advanced prostate cancer may lead to bony pain, weight loss, trouble voiding, blood in the urine, or kidney obstruction.
Prostate cancer incidence increases with age, majority of prostate cancers are diagnosed after the age of 65.
Men whose relatives have had prostate cancer are considered to be at higher risk than the general male population.
Men with high PSA levels at a young age are at higher risk of developing and dying from prostate cancer. Men in the highest 10% of PSA concentrations at the age of 45-55 will contribute to approximately half of prostate cancer-related deaths occurring before the age of 70-75.
Diagnosis of Prostate Cancer
Prostate cancer screening involves performing a PSA (prostate specific antigen) blood test and a prostate examination by a doctor through the rectum. PSA testing combined with DRE helps identify prostate cancers at their earliest stages.
PSA is a protein that is produced by normal cells as well as cancerous cells of the prostate. Prostate cancer cells generally make more PSA then do non-cancerous cells. It is known that PSA blood test is not perfect as a prostate cancer screening tool, but then used with other information and data can be helpful to determine risk of prostate cancer.
Other important variables in regards to prostate cancer screening are a gentleman’s age, family history of prostate cancer, the size of the prostate, and how quickly the PSA is changing over time.
An elevated PSA can have other causes, such as an enlarged prostate or prostate infection. Also, some prostate cancers produced low levels of PSA due to the cancer cells changing rapidly and becoming less capable of secreting the PSA protein.
Some prostate cancers are slow growing such that no treatment is initially recommended and surveillance is carried out with follow-up office visits. Other prostate cancers pose risk to a man’s longevity and treatment is recommended.
There are pros and cons of prostate cancer screening that should be discussed with your doctor. In addition, other diagnostic tools have emerged over the past several years to assist in determining risk for prostate cancer. Your doctor can review these tests with you if they seem appropriate for your situation. Overall, the goal of prostate cancer screening would be to detect a clinically relevant prostate cancer in a man with many years of active life ahead of him. Most medical organizations encourage discussion of the option of prostate cancer screening in men at age 50.
At times a biopsy is recommended for evaluation for prostate cancer. This is typically an office procedure that takes about 15 minutes and involves placement of a transrectal ultrasound probe to view the prostate. A local anesthetic is placed near the prostate to numb the area prior to a biopsy. Tiny biopsies are taken of the prostate, usually 10 or 12, and these are evaluated by a pathologist under a microscope. Men are usually asked to take it easy that day. Reports usually return in 5-7 days. Risks are generally low, but include infection of the prostate, rectal bleeding, or urinary retention. At times, a transperineal biopsy is recommended to access an area of the prostate that may be more difficult to access with the transrectal approach.
When a biopsy confirms the presence of cancer, the pathologist examines a sample of your cancer to determine how much cancer cells differ from the healthy cells. A higher grade indicates a more aggressive cancer that is more likely to spread quickly. The most common scale used to evaluate the grade of prostate cancer cells is called a Gleason score. Scoring combines two numbers and can range from 6 (low-risk cancer) to 10 (high-risk cancer).
Treatment of Prostate Cancer
Many treatment options are available for prostate cancer. Prostate cancer treatment is tailored to the patient’s needs, taking into account the aggressiveness of cancer, the degree to which cancer has spread and the general health of the patient.
Possible treatment options include:
Active Surveillance
For men diagnosed with a small volume of low-risk prostate cancer, treatment may not be necessary right away. Some men may never need treatment if the prostate cancer remains low grade. Instead, doctors may recommend close monitoring of the prostate cancer using regular PSA, MRI scans and sometimes biopsies to monitor the progression of prostate cancer. If tests show your cancer is progressing, you may opt for curative prostate cancer treatment such as surgery or radiation.
Radiation Therapy
Radiation therapy uses high-energy photons to destroy cancer cells.
This can be delivered from outside of the body (external beam radiotherapy) or using radioactive seeds placed into the prostate gland (brachytherapy).
External beam radiotherapy usually involves a 10-20 minutes session of treatment five days a week for 5-8 weeks. Your doctor may place gold markers within the prostate gland to improve the accuracy of radiotherapy targeting. Your doctor may also inject a gel called SpaceOAR between the prostate and the rectum to protect the rectum from being affected by radiation.
Side effects of radiation therapy can include painful urination, frequent urination, and urgent urination, as well as rectal symptoms, such as loose stools or pain when passing stools. Erectile dysfunction can also occur.
Hormone Therapy
Prostate cancer cells require testosterone (male hormone) to grow. Without testosterone, cancer cells die or grow more slowly. Hormone therapy reduces the levels of testosterone in the body. This can be administered by injections administered every 3 months or permanent surgery to remove the testosterone-producing cells in the testicles.
Hormone therapy is used in men with advanced prostate cancer to shrink cancer and keep it in check. In men with early-stage prostate cancer, hormone therapy may be used before radiation therapy. This can make it more likely that radiation therapy will be successful.
Surgery to remove the Prostate – Radical Prostatectomy
Surgery involves removing the prostate and seminal vesicles and then reconnecting the bladder to the water pipe (urethra). The surgeon may elect to preserve the nerves around the prostate gland in order to preserve erectile function in suitable patients with prostate cancer that is localized within the prostate gland. In patients with more aggressive prostate cancer, the nerves and surrounding tissues around the prostate gland are also removed to ensure complete removal of all cancer cells.
Robotic Assisted Laparoscopic Radical Prostatectomy
Four robotic arms are inserted into the lower abdomen through several small incisions. The surgeon controls the robotic arms from a console next to the patient. The robotic device allows a more precise and dexterous response to movement of the surgeon's hands. This technology allows reduced pain, less blood loss, less scarring and a quicker return to normal activity for the patient.
